- Charlie Camosy, OSV News
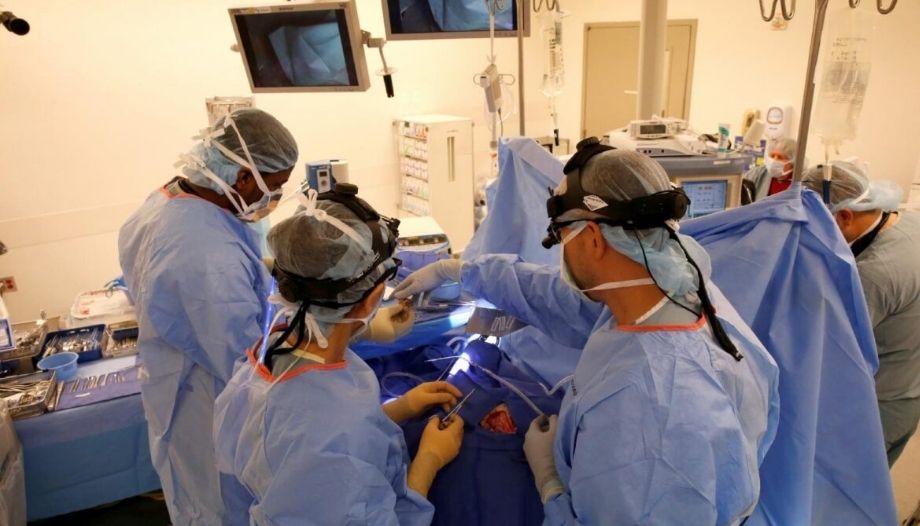
An important area of study and research is now in the field of neurotechnology, which is closely related to neurosurgery. Brain-machine interfaces have the potential to help patients with debilitating conditions, such as total quadriplegia, to regain significant autonomy.
The idea is that the brain is healthy in this group of patients. The pathology they suffer affects the connections of the brain with the rest of the body.
We talked about it with Gabriel LeBeau, a second-year neurosurgery resident at the University of Kansas Medical Center, who has been thinking about brain bioethics for some time, and is interested in brain-machine interfaces, neurotechnology, and cerebrovascular neurosurgery.
Charlie Camosy: Can you tell us a little bit about your Catholic journey and how it led you to do a residency in neurosurgery?
- Gabriel LeBeau: I was born and raised Catholic, especially in the Catholic Charismatic movement. My family was devout and I am deeply grateful to my parents for fostering the gift of faith.
I grew up in Arizona, but chose to attend college at Benedictine College in Atchison, Kansas. This college experience deeply solidified my Catholic identity and united my desire for excellence with the Catholic intellectual and moral tradition. I studied philosophy, also studied medicine and had always been attracted to biomedical ethics.
As I progressed in my studies of philosophy, philosophical psychology, the questions of free will, the difference between brain, mind and soul, mind-body duality, etc., were the ones that grabbed me the most. I was fortunate enough to be accepted to the University of Kansas Medical School, and it was these philosophical interests that propelled me into brain-related specialties.
While in medical school, I was fortunate to be mentored by a deeply Catholic neurosurgeon, Dr. Paul Camarata. He helped foster and support my interests in neurosurgery, as well as my Catholic identity in that field. His care for patients, commitment to faith and operational excellence gave me the confidence to pursue neurosurgery as my specialty of choice.
How do you define neurosurgery?
- Neurosurgery is a surgical specialty that deals with pathologies and emergencies affecting the central and peripheral nervous system, i.e. the brain, spine and nerves. Patients present with symptoms that affect their sense of identity, autonomy and many other factors central to the human condition. Often, these pathologies appear without warning and in the context of an emergency, and can be fatal or life-changing without intervention.
I believe that the Catholic moral tradition, guided by the spiritual and corporal works of mercy, is essential to my future training and practice as a neurosurgeon in the care of these patients and families.
Brain-computer interfaces, potential for patient support
Thank you for joining our team at the Institute for Advanced Catholic Studies at the University of Southern California. Can you share a brain-related idea you've had from our time together?
- It is difficult to share just one brain-related idea, because there have been so many. One that comes to mind is especially related to brain-computer interfaces. The group in question is studying the philosophy (or movement) of transhumanism and its impact on multiple fields.
One area of impact would be in the field of neurotechnology, which is closely related to neurosurgery. Brain-machine interfaces have the potential to help patients regain autonomy.
Through a brain-machine interface, a device can be implanted in the brain, which in turn would collect and synthesize neural data in a computer to produce an actionable output, such as moving a robotic arm or having autonomy over the actions of a computer or other device.
There are many models of this with early success, such as patients regaining ownership of their businesses, operating prostheses and many other exciting developments.
A situation that was once intractable now enters the realm of neurosurgical intervention. Prominent industries involved in this sector are Neiuralink and Synchron.
These innovations can be used for many purposes.
- As with many technologies, this innovation can be used for many purposes. In current models, brain-computer interfaces are intended to restore patient autonomy and improve quality of life in what was once considered an untreatable condition.
However, these same devices, with the same technology, could be used with a ‘transhumanist’ mentality, in order to implant these devices in a healthy patient with the intention of improving them.
This team has examined the philosophical and ethical implications of such use and, importantly, has collaborated with both academic and industry leaders in the world of neurosurgery, achieving a successful interdisciplinary dialogue. The neurosurgical field is becoming aware of the ethical implications of these devices because of the work of this group.
As you know, I have been asked about the relationship of the brain to self-awareness and, ultimately, to human life and death itself. Do you think there are questions worth asking here?
- Yes, indeed. There seems to be a bias in the scientific and medical community that the brain and the mind are synonymous. Given this assumption, the perceived value of a person often rests on the functionality of his or her brain.
Philosophically, there are important questions to raise here, namely, whether it is true that brain and mind are synonymous, and how best to characterize that relationship.
Many books have been written addressing this very question, but I can comment that in the operations I assist in as a resident (awake brain tumor surgeries, seizure resections), large and important parts of the brain can be removed, and the mind seems to remain intact after the operation.
However, in practice, I see the implications of the idea that a person's brain, mind and worth are synonymous most poignantly in the delineation of ‘brain dead’ and the rationale for that classification in the first place.
Sometimes you want to manipulate responses
A related issue worries me: that we have become lazy and inaccurate in thinking about the question ‘What is death?’ partly because we want to manipulate the answer to get more organs for transplants....
- From the outset, I would argue that “brain death,” or “death by neurological criteria,” in our experience has no real clinical utility beyond organ procurement.
In the field of neurosurgery we encounter many patients and their families after neurologically devastating injuries. Once all options are presented to the family, whether to have surgery or not, decisions are made without “brain death” to withdraw extraordinary care and allow their loved one to succumb to the natural process. Brain death testing is of no help at all in this process at our hospital, in almost all cases.
Now the conversation about brain death comes in. In every hospital in the region, for every patient who meets certain neurological presentation criteria-I think in our hospital it's Glasgow Coma Scale of five or less-the local organ transplant network receives automatic notifications.
We assume that the organ donation industry is also concerned with.
- Occasionally, although rare, the organ procurement representative speaks to the family before the physician has a chance to do so. I have heard a speech by a representative in a situation where a young man attempted to take his own life with a gun to his head, in which it was said, “your son's death may mean something.” This is not physician driven, nor do many physicians of all faiths appreciate the enthusiasm of the organ procurement industry.
Other concerns I have are addressed in the medical literature, including. works published in The Annals of Thoracic Surgery and The American Journal of Transplantation.
A comment on the moral certainty of death.
- It is important to note that there are active efforts to “maintain the principle of permanence of death” in donation after circulatory death (Note: in medicine this principle coincides with the Catholic requirement of irreversibility and moral certainty of death before proceeding with donation).
In this case, the patient dies of cardiac arrest and is declared dead. When resuscitated for surgical removal, major cerebral arteries are clamped, with the idea that the person will maintain the permanence of death by impeding blood flow to the brain.
There are aspects of the organ donation industry and of the transhumanism that are controversial and should be carefully analyzed.
(You can consult the Catechism of the Catholic Church, nn. 2292-2296, concerning ‘Respect for the person and scientific research’).
——————–
- Charles Camosy teaches moral theology and bioethics at The Catholic University of America in Washington.